VytlOne
VytlOne has over 30 years of experience and an award winning customer service team that will be available for 24/7/365 support.
A new Drug Search tool is available to SmartHealth members. This tool will allow members to search medications to determine the formulary tier, drug class coverage, and if a prior authorization is required.
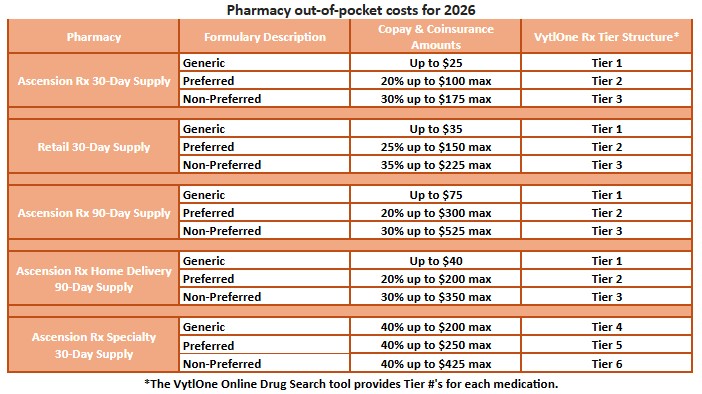
Pharmacy out-of-pocket costs for 2026
Pharmacy Benefit Details
Important pharmacy benefit and ID card information
A new pharmacy ID card will be sent to you for VytlOne's drug plan in the beginning of the year. Please note that this card is different from your medical card. To fill prescriptions, you must use your new prescription ID card.
If you need a new card, please call 888-492-6811 or download the Ascension One app to access a digital copy of your card.
Important pharmacy documents
-
Maintenance medicationsMaintenance medications are medications taken at home on a consistent schedule to treat chronic or long-term conditions. This may include oral, injectable, inhaled, ophthalmic and topical medications. Specialty medications are not considered maintenance medications within your pharmacy benefit. These two classifications have different definitions and requirements within SmartHealth. Learn more about maintenance medications including types of medications and where to fill here.
-
Ascension Rx pharmacies
-
SmartHealth Specialty Prescription Drugs
SmartHealth specialty prescription drugs are Tier 4, 5 and 6 on this online drug search tool
A specialty medication is considered a high-cost drug used to treat complex conditions. These drugs are available from your pharmacy benefits, and are usually self-administered. Specialty medications are prescription drugs that are filled by a specialty pharmacy because they have requirements that can only be fulfilled within our Exclusive Specialty Pharmacy Network. Specialty medications meet or exceed a cost of $830 for a 30 days supply, require special handling, require additional patient education, and/or require clinical pharmacy intervention to ensure safe use of the specialty drug.
Specialty medications must be filled within our Exclusive Ascension Specialty Pharmacy network. Some medications may be subject to participation in the Flexible Copay program.*Information on the Flexible Copay program appears below on this website. -
Manual claim forms
This claim form can be used to request reimbursement of covered expenses paid out of pocket.
-
Continuous glucose monitors
Continuous glucose monitors (CGM) are important tools for tracking and managing diabetes. Your plan offers coverage for the Dexcom CGM sensors & transmitters under your pharmacy benefit. The Dexcom CGM is available by prescription from your provider, and does require prior authorization. Prescriptions for Dexcom can be filled at any in-network Pharmacy for SmartHealth.
-
Diabetic benefit
Ascension preferred diabetic medications and supplies receive a reduced copay when filled at an ARx pharmacy.
Medications: Novolog (additional may be added)
Supplies: T1 (preferred generic) & T2 (preferred brand)
Continuous Glucose Monitors: T2 (preferred brand)
-
Prescription Refills and Preventing Oversupply
-
2026 SmartHealth ACA ($0) Medication List
2026 SmartHealth ACA ($0) Medication List
Medications available at no cost to members under Patient Protection and Affordable Care Act (PPACA).
-
2026 SmartHealth HDHP Preventative Medication List
2026 preventative medication drug list
Preventive medications are used to help avoid disease and maintain health. For those members on a high deductible health plan (HDHP), before the deductible has been met, these medications will only be subject to copay/coinsurance and still apply towards out-of-pocket max. If your medication is not a maintenance medication on this list, continue to fill it at your local pharmacy.
Patient Assistance Programs for Prescription Drugs
SmartHealth True Spend Solutions Program for Non-Specialty Brand Prescription Drugs
The Plan includes the True Spend Program. Under this program, amounts paid by a secondary payer, such as manufacturer coupons, for non-specialty, preferred and non-preferred brand drugs will not be applied toward meeting your plan deductible or out-of-pocket maximum. You still benefit from the coupon at the point-of-sale, but your deductible and out-of-pocket totals will reflect what you actually paid.
Our Ascension Rx Medication Assistance Team can assist you with enrollment into manufacturer assistance programs for your prescription drugs. These manufacturer assistance programs can help to lower the cost of your prescriptions. The Medication Assistance Team can be reached from 8am to 4pm Central Time, Monday - Friday at 1-833-980-2352 (Press 7, then press 3).
SmartHealth Flexible Copay Program for Specialty Prescription Drugs
Every year, the cost for some specialty medications might change and go up, which means you could pay more out of pocket. To help with this, Smart Health has the Flexible Copay program. This program works with drug manufacturers' copay assistance programs to help lower your out-of-pocket costs for these expensive medications throughout the year.
However, please note that manufacturer assistance is not applied towards meeting your annual deductible or out-of-pocket expenses. For HDHP & HDHP EPO plan members, once the HDHP deductible is met with eligible expenses (e.g. medical), the member will pay the standard prescription drug copays for their SmartHealth health plan.
Please note, manufacturer assistance programs may change, or end at any time during the year. If that happens, you'll need to pay the regular copay or cost for your prescription based on your SmartHealth plan. Keep in mind that this assistance is provided by the drug manufacturer, not by Ascension Rx or SmartHealth.
If you have a specialty prescription drug with a high copay and you have questions about the SmartHealth Flexible Copay program please email our Ascension Rx Flex Copay Team at askflexcopay@ascension.org with your questions, along with your member and prescription information.
Provider administered specialty medications or infusion therapies
(Your provider or physician's office must submit the prior authorization)
All physician-administered specialty medications or infusion therapies are subject to precertification notification or prior authorization (PA) approval. For a product list with current requirements, please see the medical benefit drug list.
Have questions?
- Call 833-980-2352 to speak to a member of the Ascension Rx prior authorization team.
- Call 888-492-6811 to confirm a patient's SmartHealth plan eligibility.
To submit a precertification notification or prior authorization request for a physician-administered product or infusion therapy:
- Download the form: Medical benefit drug precertification notification and PA form
- Complete and sign the form
- Submit the completed and signed form:
- Via fax to 512-831-5499
- Via the Jiva Provider Portal at https://bit.ly/AscensionProviderPortal